There Could be a Problem with Sparkling Water
The relationship between carbonated beverages and weight management is more complicated than most dietary guidance acknowledges. The explanation provided here runs much deeper than calories, sugar content, or ingredient labels. This article presents a systems-level examination of how carbonation (including sparkling water), regardless of caloric content, interacts with the hormonal architecture governing hunger, the stress response, and fat storage.
I am writing this for two audiences. The overview below provides an at-a-glance view of the essential argument. For those wanting to dig deeper, a fuller mechanistic case is developed throughout.
Article Overview
- Mainstream outlets will tell you that sparkling water will not cause weight gain. However, all carbonated beverages, including sparkling water, stimulate the hunger hormone (ghrelin) through gastric pressure. But ghrelin also initiates a hormonal cascade involving cortisol and insulin that the zero-calorie label and mainstream research do not account for.
- The downstream effects linking carbonation to ghrelin, ghrelin to cortisol, and cortisol to epigenetic fat-storage pathways are each independently supported by existing research. However, this article is somewhat novel because it appears to be the first time that the complete chain has been offered as a unified system.
- People stalled in their weight-loss journey who have already eliminated soda in favor of sparkling water may find that removing carbonated beverages entirely is the variable their plateau has been waiting for. Try eliminating all carbonated beverages for 4 to 6 weeks and see how you look and feel.
Sparkling Water Isn’t Neutral
For millions of people navigating a weight-loss journey, the advice sounds reasonable enough: ditch the soda, switch to sparkling water. At face value, it seems logical. You eliminate the syrup, the refined sugar, the empty calories, and the inflammation-driving glucose load that comes with regular soft drink consumption. By nearly every conventional metric, the swap represents genuine progress. And it is progress, but only to a point. The problem is that progress is not the same as a solution, and understanding the difference may be precisely what people who have stalled need to hear.
The dominant framework in weight management remains stubbornly caloric. Consume less than you expend, the model insists, and the weight comes off. To demonstrate why this thinking is flawed, I’m using sparkling water as a useful example, precisely because it appears to satisfy the model completely: zero calories, no sugar, no syrup. And yet, results can remain elusive, and other conditions can spring up. We must understand that the human body does not respond to food and drink through a single variable. It responds through systems. Sparkling water is simply a clean case study for a much larger problem with how we think about consumption and metabolic consequences. So, let’s dig in by examining sparkling water through a health science lens.
Carbonation, the Stomach, and the Hunger Signal
When a carbonated beverage enters the stomach, two things happen almost immediately. First, the carbon dioxide expands into a gas, and the resulting pressure stimulates mechanoreceptors in the gastric lining. Those mechanoreceptors then communicate with a network of enteroendocrine cells, and among the signals the network generates is the release of ghrelin, a peptide hormone most commonly known as the “hunger hormone.” Granted, research in this area is limited, but the finding itself has emerged with enough consistency to warrant attention. What you need to know here is that carbonation, independent of caloric content or sugar load, appears to stimulate ghrelin secretion.
Now, for someone trying to lose weight, a ghrelin spike is already an unwelcome development. Elevated ghrelin signals the hypothalamus to increase appetite and promote food-seeking behavior. It stimulates neuropeptide Y and agouti-related peptide neurons in the arcuate nucleus, which in turn suppresses the satiety signals the body would otherwise generate. This means that your zero-calorie beverage may be working against the appetite regulation you’re trying to maintain. Ultimately, this means you are likely to eat more. But there’s a bigger problem. Ghrelin does not operate in isolation, and this is where the conversation becomes more consequential… and seems to be entirely overlooked.
There is a Downstream Problem, Though
Again, since the body is a system, we must think in systems. Let’s start with the idea that ghrelin is a systemic signaling molecule with receptors far beyond the gut. One of its primary targets is the anterior pituitary, where it stimulates the release of adrenocorticotropic hormone (ACTH). ACTH, in turn, drives the adrenal cortex to produce cortisol. This is a documented axis. However, in practical terms, this means that a ghrelin spike does not remain confined to hunger signaling. It has a plausible and mechanistically supported route to elevating cortisol.
Cortisol’s relationship to weight, particularly abdominal adiposity, is well established in the literature. What is less commonly discussed in popular health circles is how cortisol influences gene expression. Glucocorticoids, the class of hormones to which cortisol belongs, bind to glucocorticoid receptors that function as transcription factors, thereby directly influencing which genes are expressed and which are silenced. That can get a little complicated, but the point is that among the pathways cortisol can activate through this mechanism are those governing adipogenesis, the biological process by which precursor cells differentiate into fat-storing cells. What you need to know here is that repeated cortisol elevation, even at moderate levels, has been associated with epigenetic modifications that shift the body’s metabolic set point toward storage rather than expenditure.
Of course, ghrelin also antagonizes insulin directly, suppressing secretion from pancreatic beta cells while simultaneously stimulating glucagon from alpha cells. Well, the net effect is a push toward hepatic glucose output and reduced peripheral glucose uptake. Granted, a single beverage is probably inconsequential. However, repeated across dozens of daily sparkling water servings over weeks and months, the cumulative hormonal environment tilts in a direction that calorie math alone cannot explain. The downstream effect is a body that is being encouraged to store whatever extra it can find. Hence, weight gain or weight loss stalls.
However, if that wasn’t enough to make you think twice about carbonated drinks, perhaps this will. Not all brands are created equal, and you never truly know what you’re going to get. Concerns have recently emerged about PFAS, or “forever chemicals,” being detected in some sparkling water brands. These synthetic compounds resist heat, water, and oil and are widely used in products such as food packaging and textiles, but their persistence has raised legitimate health concerns in recent years, including elevated cholesterol levels, impaired immune response, and even kidney and testicular cancer (Buera, 2024).
Of course, this also means that some sparkling water brands may contain compounds that interfere with the body’s hormonal signaling architecture, well beyond appetite regulation. That’s because PFAS have also been shown to disrupt thyroid hormone function, alter estrogen and androgen activity, and interfere with insulin signaling pathways (Di Nisio et al., 2022). In other words, the same drink that may be triggering a ghrelin-mediated hormonal cascade could simultaneously be introducing synthetic compounds that compound that disruption through an entirely separate mechanism.
For someone already struggling to lose weight, that compounding effect is a problem. After all, the body’s endocrine system is not a collection of isolated switches. It is an integrated signaling network, and when multiple inputs push it in the same direction simultaneously, the downstream consequences become increasingly difficult to attribute to any single cause. That is precisely why people stall, why the etiology of some conditions remains elusive, and precisely why the recommendation to simply swap soda for sparkling water deserves more scrutiny than it typically receives.
A Practical Recommendation for the Stalled
For those who have made genuine dietary progress, reduced their caloric intake, eliminated soda, reduced refined sugar consumption, brought inflammation down, and maybe even implemented Nature’s Intent to the fullest, but their weight loss has plateaued in ways you cannot otherwise explain, carbonated beverages are a reasonable variable to eliminate and observe. I should be clear that the recommendation here is not that sparkling water is equivalent to soda. It is not. The caloric reduction, the elimination of refined sugar, and the reduction in systemic inflammation that comes from removing conventional soft drinks are real benefits. The recommendation is simply that “zero calories” does not mean “zero hormonal consequences,” and for some individuals, particularly in certain metabolic states, that distinction may be exactly what the plateau is trying to communicate.
If that describes the situation, simply try removing carbonated beverages entirely for 4 to 6 weeks and replacing them with spring water, herbal teas, or some other non-carbonated, zero-calorie options. Monitor not just weight but appetite patterns, cravings, and energy consistency. Those are important. The body communicates through those variables, too. And most importantly, remember that these communications often shift before the scale does.
Of course, the broader lesson here applies well beyond this single dietary question. This is merely one example of many. The point is that reducing complex biological systems to one measurable variable, whether calories, macronutrients, or any other single marker, will always leave explanatory gaps. Those gaps are where stalled progress lives. Thankfully, thinking in systems does not require a graduate degree in endocrinology. It simply requires the willingness to ask what else might be happening and the discipline to follow the logic wherever it leads.
What the Research Does and Does Not Say
What has been presented here is admittedly speculative, but it is also absolutely defensible. However, intellectual honesty requires acknowledging the limits of the available evidence. Yes, the studies examining carbonation and ghrelin are small, and some might see this idea as rather novel. After all, no formal population study has traced the complete chain from carbonated beverage consumption to ghrelin elevation to cortisol to epigenetic modification of adipogenic pathways in a single human cohort. That would probably be somewhat difficult. That said, the clinical observation of individuals who have stalled in their weight-loss journey despite meaningful behavior change, including the elimination of conventional soft drinks, is itself a data point worth taking seriously.
Regardless, what can be said with confidence is that each link in that chain is independently supported by existing research. For example, the ghrelin–ACTH–cortisol connection is well documented (Azzam et al., 2017; Giordano et al., 2004; Schmid et al., 2005). Cortisol’s capacity to modify gene expression in adipogenic pathways has been documented (Campbell et al., 2011; Lee, Harris, & Wang, 2018; Wan et al., 2024). The ghrelin-insulin antagonism is documented (Meyer, 2010; Tong et al., 2010). Gastric mechanoreceptor activation by carbonation and its downstream hormonal effects are documented, if understudied (Eweis, Abed, & Stiban, 2017; Pouderoux et al., 1997). Well, if we put the pieces together, it probably looks something more like this:
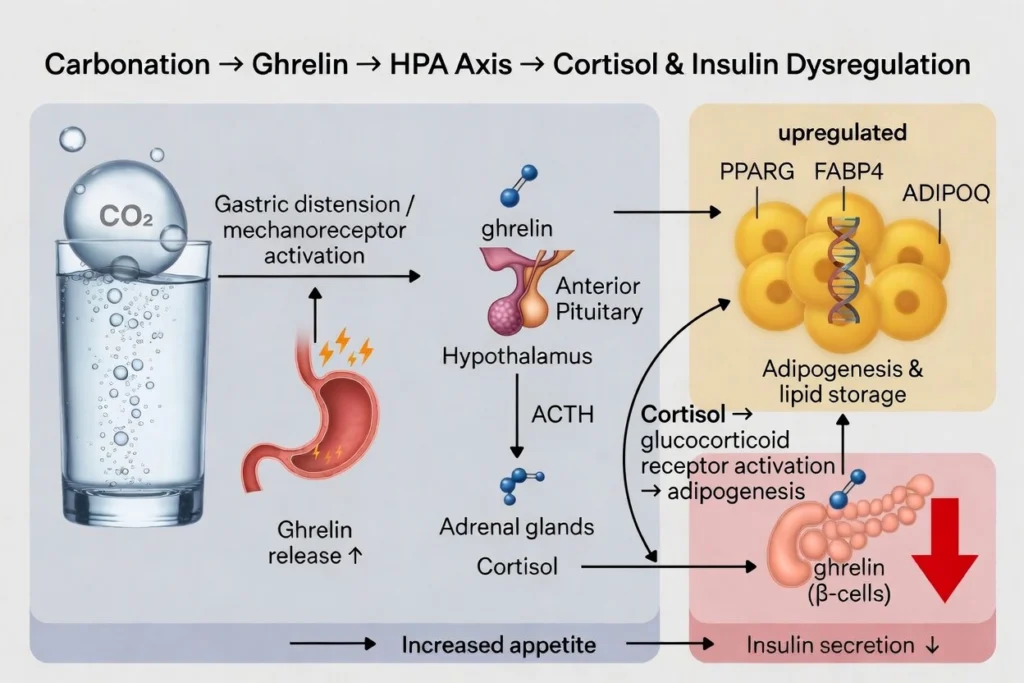
Understand my motive here. I am not trying to stir the pot. This article simply presents the systems argument as a logical assembly of established mechanisms. The absence of a study that simultaneously connects all links is merely a gap in the literature, not evidence that the chain doesn’t exist. In fact, this would probably be a great topic for those with university funding to explore. Either way, just remember that the absence of evidence is not evidence of absence.
For me, the question is not whether this hypothesis has been proven but whether it is mechanistically plausible and whether the practical recommendation it generates carries meaningful risk. On both counts, I think it is safe to say that the answer is to take it seriously. And finally, if it matters at all, we should probably acknowledge the anecdotal evidence suggesting that when carbonation is omitted entirely, the stall often resolves. Perhaps, now we know why.
Resources
Azzam, I., Gilad, S., Limor, R., Stern, N., & Greenman, Y. (2017). Ghrelin stimulation by hypothalamic-pituitary-adrenal axis activation depends on increasing cortisol levels. Endocrine connections, 6(8), 847–855. https://doi.org/10.1530/EC-17-0212
Buera, J. (2024, July 11). PFAS in sparkling water: Should you be cautious? Nano Singapore. https://nanosingaporeshop.com/community/blog/wellness/pfas-in-sparkling-water/
Campbell, J. E., Peckett, A. J., D’souza, A. M., Hawke, T. J., & Riddell, M. C. (2011). Adipogenic and lipolytic effects of chronic glucocorticoid exposure. American Journal of Physiology-Cell Physiology, 300(1). https://doi.org/10.1152/ajpcell.00045.2010
Di Nisio A, Lopez-Espinosa M-J and Foresta C (2022) Editorial: Emerging Chemical Risks for Human Health: Endocrine Disruption by Per- and Poly-Fluorinated Alkyl Substances (PFAS). Front. Endocrinol. 12:813785. https://pubmed.ncbi.nlm.nih.gov/35095772/
Eweis, D. S., Abed, F., & Stiban, J. (2017). Carbon dioxide in carbonated beverages induces ghrelin release and increased food consumption in male rats: Implications on the onset of obesity. Obesity research & clinical practice, 11(5), 534–543. https://doi.org/10.1016/j.orcp.2017.02.001
Giordano, R., Picu, A., Broglio, F., Bonelli, L., Baldi, M., Berardelli, R., Ghigo, E., & Arvat, E. (2004). Ghrelin, hypothalamus-pituitary-adrenal (HPA) axis and Cushing’s syndrome. Pituitary, 7(4), 243–248. https://doi.org/10.1007/s11102-005-1173-6
Lee, R. A., Harris, C. A., & Wang, J. C. (2018). Glucocorticoid Receptor and Adipocyte Biology. Nuclear receptor research, 5, 101373. https://doi.org/10.32527/2018/101373
Meyer C. (2010). Final answer: ghrelin can suppress insulin secretion in humans, but is it clinically relevant?. Diabetes, 59(11), 2726–2728. https://doi.org/10.2337/db10-1088
Pouderoux, P., Friedman, N., Shirazi, P., Ringelstein, J. G., & Keshavarzian, A. (1997). Effect of carbonated water on gastric emptying and intragastric meal distribution. Digestive diseases and sciences, 42(1), 34–39. https://doi.org/10.1023/a:1018820718313
Schmid, D. A., Held, K., Ising, M., Uhr, M., Weikel, J. C., & Steiger, A. (2005). Ghrelin stimulates appetite, imagination of food, GH, ACTH, and cortisol, but does not affect leptin in normal controls. Neuropsychopharmacology : official publication of the American College of Neuropsychopharmacology, 30(6), 1187–1192. https://doi.org/10.1038/sj.npp.1300670
Tong, J., Prigeon, R. L., Davis, H. W., Bidlingmaier, M., Kahn, S. E., Cummings, D. E., Tschöp, M. H., & D’Alessio, D. (2010). Ghrelin suppresses glucose-stimulated insulin secretion and deteriorates glucose tolerance in healthy humans. Diabetes, 59(9), 2145–2151. https://doi.org/10.2337/db10-0504
Wan, X., Wang, L., Khan, M. A., Peng, L., Zhang, K., Sun, X., Yi, X., Wang, Z., & Chen, K. (2024). Shift work promotes adipogenesis via cortisol-dependent downregulation of EGR3-HDAC6 pathway. Cell death discovery, 10(1), 129. https://doi.org/10.1038/s41420-024-01904-9